In the present day and age we are always seeking answers from the infamous “Dr Google” for queries regarding our day to day ailments, always looking for the best possible hospital, the best possible treatment option and the best possible doctor.
However, has anyone ever wondered what was medicine like, before all the advancements and breakthroughs came into the picture?
I bet not!.
So here is an article, more like a time machine that will take you back in time and will give you an insight into the field of medicine what was it like in the past and how it is at present.
Revisiting The Past
In the past, it was thought that the human heart had only 2 chambers and many did not know what its exact function was.
In the 2nd century, a Roman Physician by the name of Galen was the first to come up with this theory. He said that the human heart was in fact a source of body heat. He published this in his book which became a worldwide bestseller, however nobody at that time questioned his findings.
It was only in the year 1543 that Andreas Vesalius, an anatomist, disproved Galen’s theory after studying various corpses. He revised Galen’s findings and said that the heart in fact had 4 chambers and not 2.

However the exact function of the heart was still under debate at that point of time. Vesalius is now considered as the father of modern human anatomy.
Another turning point in medical history was the year 1648.
This was the year when William Harvey concluded his experiments on various animals and translated his data on humans.
Contrary to popular belief at that time, he theorized that the heart is in fact a pump !!
He spoke about the arteries and veins in the body and even talked about how blood flowed in a “circle” in the body. This explanation changed how treatments of ‘blood removal’ were being done back then.
I am sure you must be aware of the terms ‘systole’ and ‘diastole’. You must have heard a lot of medical professionals use the same. These are terms used to describe blood pressure.
Systole is the first number in the blood pressure reading, while diastole is the second number.
But back when techniques were redundant, how could one tell the difference between the two?
The credit for this goes to a French physician, Rene Laennec.
In the year 1817, he invented the stethoscope and introduced the ‘auscultatory‘ method (or listening method) to measure blood pressure.
The story behind his invention is actually quite fascinating.
One day a young female patient, with a known heart condition came to his office. However due to her age and sex he was unable to listen to her chest.
This was because doctors used to place their ears directly onto the chest to listen to the heart. This would be inappropriate for him to do.
To overcome this issue, he recollected a simple acoustic principle – scratching of the pin on a piece of wood at one end can be heard distinctly when our ear is placed at the other end.
Envisioning this, he rolled a piece of paper and placed it on the patient’s chest & voila! – the first ever stethoscope came to be.

We all know that our country was plagued with polio and unfortunately millions succumbed to the disease.
This is because this condition affects the muscles of the diaphragm, an integral part of our respiratory system that allows us to breathe in and out.
During that era, the west had come up with a solution to prolong survival in patients suffering from the disease.
The device used was known as the “Iron Lung”.
This device used the principle of negative pressure and respiratory system dynamics to counter respiratory muscle paralysis and improve air exchange.
The first one was used for an 8 year old child who was suffering from polio at Boston Children’s Hospital in the year 1928. Patients were placed in this device with their whole body enclosed except their head.
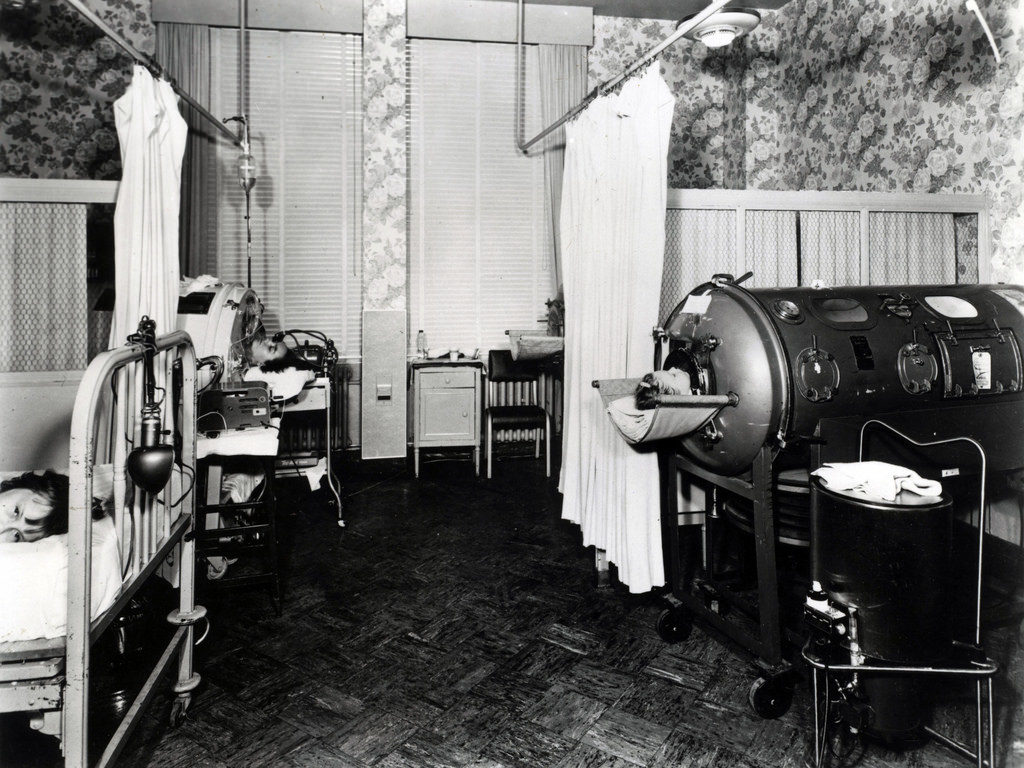
The next breakthrough in the medical field is a device that is commonly used at present by most of the patients.
It is related to a disease of the modern era, by now I am sure you know what I am talking about.
Yes!
It is diabetes and the breakthrough invention is the glucometer, which has become an integral part of countless lives.
But have you ever wondered about the history of the glucometer?
So, it all started out in the late 60s and early 70s. The initial method to measure blood glucose was by using strips of paper and watching for colour change.

The colour was then compared to a standardized chart and would give a result whether the glucose level in the body was high, low or normal. It did not provide an exact value as we receive today.
It was only in the year 1970 that the first glucometer came into existence. These glucometers used the reagent strips mentioned above and would check for the reflection of light from the colour change that occurred after the strip had been exposed to the patient’s blood sample.
However, these were not portable and were electrically powered, which meant the patient would have to come to the doctor’s office every single time.
It was only in the year 1981 that the first portable glucometer was invented, this was much better than the previous models because the waiting time to receive results was significantly reduced and blood sugar levels could be measured at home.
So What’s Exciting Now?
Imaging studies currently have reached a whole new level. Every year the detail provided by the instruments keeps getting better and better, it also aids in diagnosing complex conditions which would have been difficult to diagnose in the past.
For instance, we now have instruments that can give us a 3 dimensional image of the structure we would like to examine. Echocardiography machines can now provide 3-D images of the heart which are invaluable during heart surgery.
There have also been advancements in the field of nuclear medicine which allows us to visualise finer details of different parts of the body.
Gone are the days when imaging modalities gave us a static picture of the organ in question. Now, while performing the diagnostic test, we can assess how the organ functions in real time.
A simple instrument like the stethoscope has also undergone several modifications.
3M and other major companies have introduced digital stethoscopes with sound amplifiers. These help us to listen to the heart better and help us identify those nagging murmurs which might have been missed previously.
Ventilators used in hospitals and ICU settings have undergone a lot of advances too.
For instance, the “Iron Lung” mentioned earlier was based on negative pressure ventilation, meaning the air was removed from the lungs.
However the current instruments uses positive pressure, meaning air is pushed into the lungs.
Providing ventilation to patients is shifting from invasive methods to non-invasive methods. This means that tubes being shoved into the throat of patients is now reducing.
This has helped reduced the incidence of ventilator associated lung injuries due to excess and repetitive application of positive pressure to maintain a patent airway.
Good news for patients with diabetes!!
A new glucometer which measures glucose non-invasively has now been launched in the United States.

This means you don’t have to constantly prick your finger to measure your blood glucose levels. It uses a sensor which can be worn over your arm and it monitors your glucose levels in real time.
All you have to do is just tap the glucometer on the sensor and this would give you your current glucose levels, glucose levels in the last 8 hours and its trend.
The sensor is water resistant and can be worn anytime. The glucometer will give you an accurate reading even if the sensor is placed below clothing.
Pretty cool isn’t it!!
This is being introduced because of the increasing trend for continuous glucose monitoring, as blood sugars are controlled better and dosing for insulin can be adjusted accordingly. It is not yet available in India.
I hope this article gave you a good review of how medicine has evolved from the past and how it is making the lives of patients and doctors much simpler at present.


News about new glucometer which measures glucose non-invasively is quite interesting and welcome. I wish it is introduced in India very shortly.
Very good for lay men like me, he is fit to be an academician in his field. Thank you.
I am amazed at the ancient iron lung machine. Woahh!